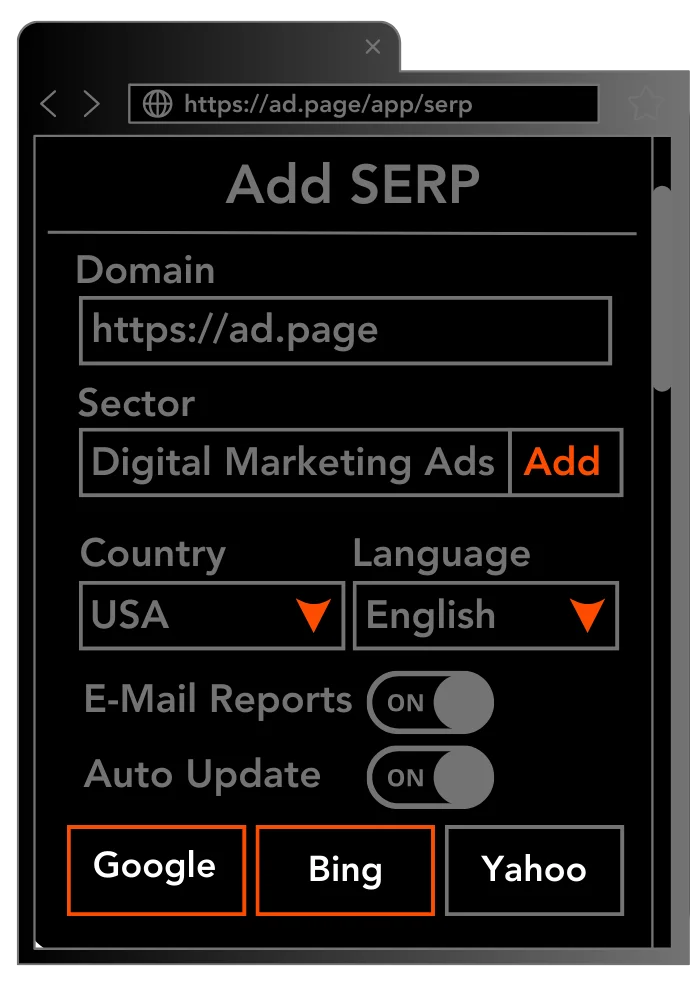
Page SERP Checker
Page SERP is an advanced SEO analytics tool for websites. It provides detailed insights into how websites are performing in popular search engines such as Google, Bing, and Yahoo. By using Page SERP, webmasters can track a variety of data points related to their websites, including rankings for specific keywords, click-through rate, and more.
In addition, Page SERP also offers advanced features such as global location targeting, device type filtering, and multiple search type results. It provides users with detailed API documentation in order to help them make reliable integrations with the Page SERP platform. With its scalable and queueless cloud infrastructure, Page SERP allows users to make high-volume API requests with ease or you can use directly from Dashboard.
Features
-
Get quick access to real-time SERP Checker data from popular search engines like Google, Bing, and Yahoo.
-
Monitor website performance with structured data analysis including page titles, descriptions, and content ranking.
-
Understand how the competition is doing by tracking competitors’ SERP ranking and tracking their performance.
-
Easily pinpoint areas of improvement by identifying key SEO issues, such as missing page titles, duplicate content, and low keyword rankings.
-
Optimize websites for specific regions or cities with geographic SERP data.
-
Unlock more efficient process automation with APIs to integrate SERP data into webmaster tools.
-
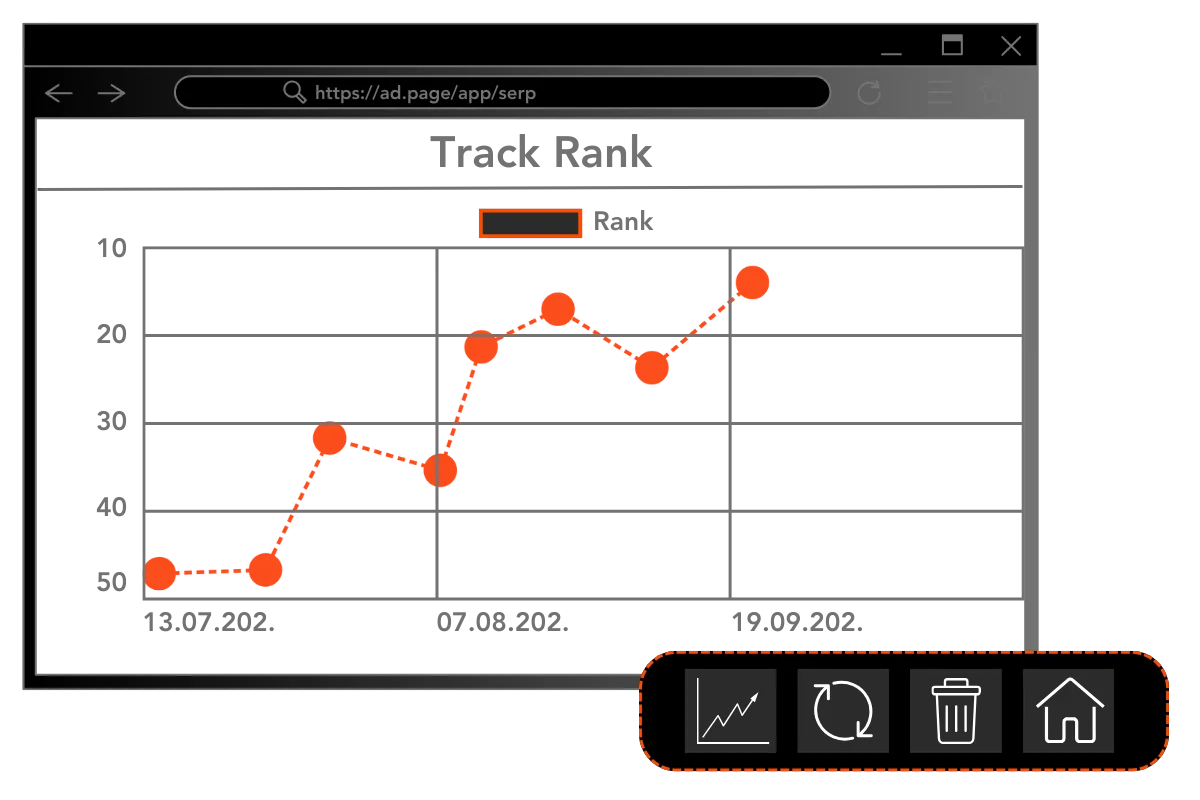
Track the progress of SEO campaigns with detailed reports and charts.
-
Access data anytime from anywhere with global coverage and device types to accommodate any SEO campaign.
-
Benefit from improved site performance with the right SERP analytics tool.
-
Enhance search engine visibility with accurate SEO analysis and real-time data.d ensure they are getting the most out of their website.
Integrated Search Engines
Yahoo
Bing
Search Engine Integrated: Search Engine Integration allows you to obtain data from popular search engines and use it for a variety of purposes. SERP Seo analytics tool for websites gives you access to website data from Google, Bing, Yahoo, and other major search engines.
By integrating these search engines into your website, you can track the performance of your website in terms of ranking, traffic, and other statistics that matter to you. This data can then be used to improve your website‘s SEO ranking and boost website traffic.
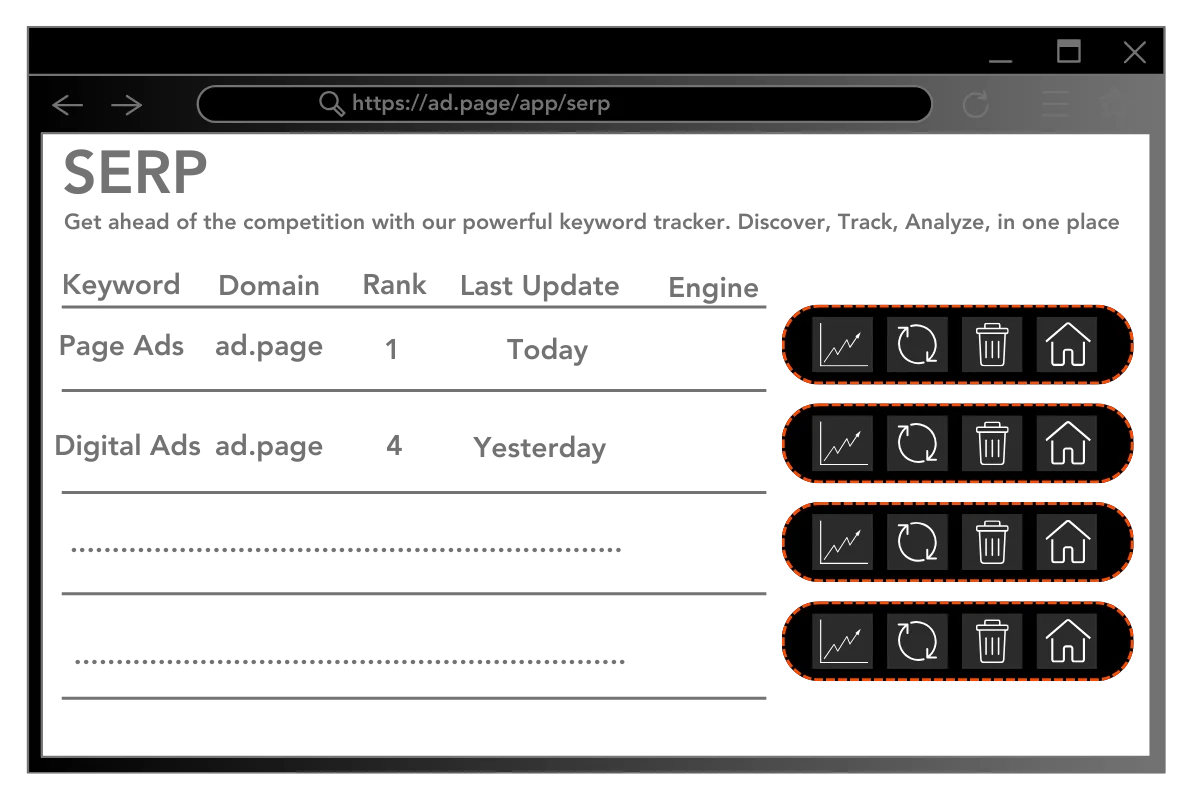
All-In-One SERP Service
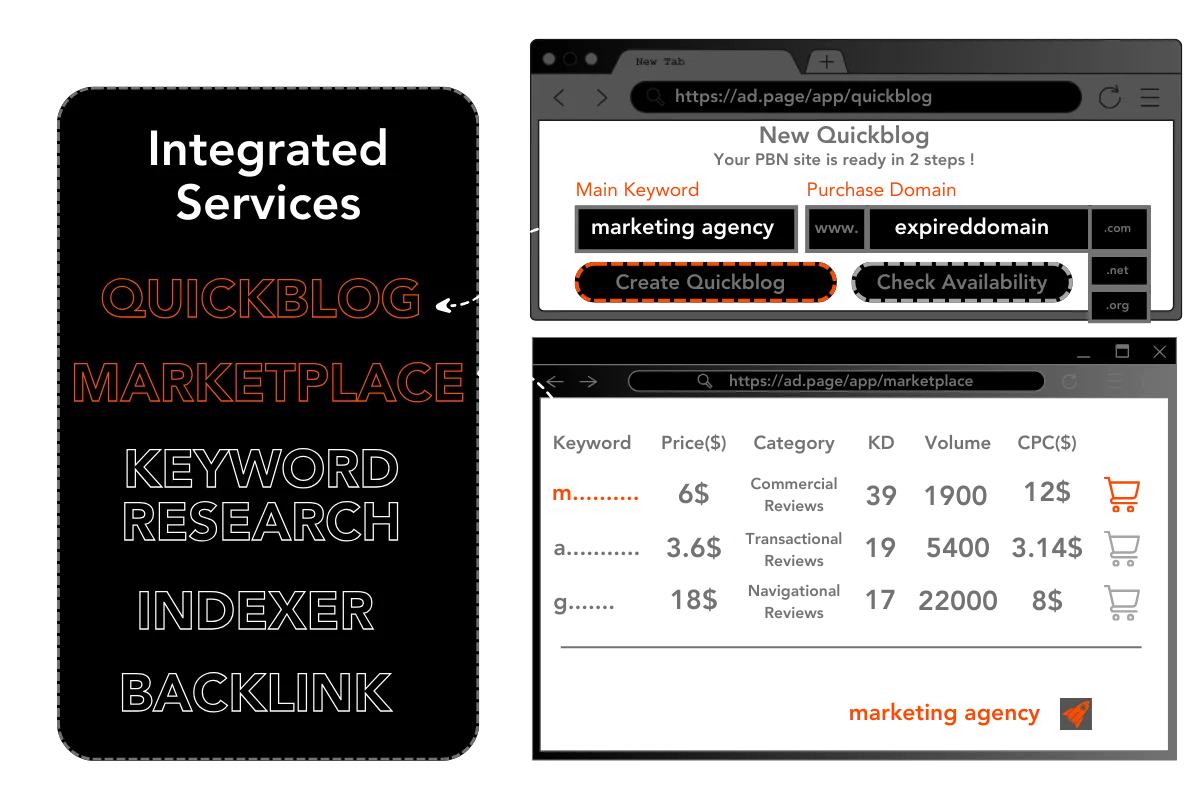
Real Time Results
Realtime SERP analytics is becoming increasingly important for webmasters to stay ahead of the competition and get the most out of their online presence. SERP Page provides the latest and most accurate data directly from popular search engines, giving webmasters the most detailed insights into their ranking performance and helping them identify opportunities to improve their ranking.
The realtime results provided by SERP Page allow webmasters to analyze their website and optimize their content in real–time. Thanks to SERP Page’s accurate and detailed data, webmasters can make informed changes to their website’s content to improve their ranking and visibility in search results. Additionally, SERP Page offers device–specific data, allowing webmasters to tailor their optimizations for specific devices. This data can also be used to inform content and conversion rate optimization in general.
Aditionally, webmasters can leverage SERP Page’s cloud infrastructure to access data without having to wait on queues. This can ensure that data requests are completed in an efficient and timely manner and help ensure that webmasters always have access to the latest insights.
Overall, SERP Page provides a powerful analytics tool that can help webmasters get realtime, detailed insight into their online presence. This data can help webmasters make informed decisions anRealtime Results and Benefits for Webmasters: